
The bright fluorescent lights and cold air sliced through the operating room. No soft lighting from the lamp on the nightstand. No gentle breeze from bedroom ceiling fan. No walks in the backyard under the giant oak tree through hours of labor. An emergency C-section. She wasn’t supposed to be born this way.
I shook uncontrollably, stuttering over my words. The nurses wrapped a warm blanket around me and had me lay down while they continued darting around.
The anesthesiologist asked if I had any music requests. I was going to put together the perfect playlist, but at four weeks from my due date, I hadn’t yet gotten around to it. All I could think of was Aaron Copland, and then my mind went blank. In the haze of the spinal block, I couldn’t remember my favorite piece.
Throughout my entire pregnancy, I suffered through headaches, backaches, and colds without any painkillers or medication. For five months, I religiously logged the food I ate for breakfast, lunch, and dinner, and twice-a-day snack, impressing even the midwives. I craved avocados instead of ice cream, I learned to eat canned herring and sardines to avoid mercury and still get my omega-3s, and I drank water all day along.
After reading Henci Goer’s The Thinking Woman’s Guide to a Better Birth and Ina May Gaskin’s Guide to Childbirth, talking to other women who had home births, and weighing the risks—including my first obstetrician’s warning that either baby or I could die—my husband, Daniel, and I were determined to have a hospital-free experience.
But baby was still breech at thirty-five weeks. I tried visualization, yoga and stretches, and visits to the chiropractor. Daniel and I tried talking to baby, playing music for baby, and shining a flashlight toward the birth canal. The midwives even tried a mild version of an external cephalic version, a procedure that involves applying extreme pressure to the abdomen to get the baby to roll head down.
When they finally gave up, they stood over the bed, holding my hand and reassuring me that I’d be in good hands with the new obstetrician who was midwife friendly. I felt as if I’d failed a big test. I could hear my old obstetrician, laughing and saying, “my way is the only way.”
I won’t lie. In a way, I was partly relieved. I’d always been secretly a little scared about doing a home birth. What if something went wrong? What if I couldn’t handle the pain? What if my baby or I would die?
On May 31, 2017, the new obstetrician scheduled me to go into the hospital, about an hour from home, to try to turn her head down once more. Although he was one of the few doctors in North Texas who was willing—and famous—for vaginally delivering breech babies, it made sense to turn her head down for an easier birth. And just like that, she turned head down, and we were sent on our way. Maybe we’d be able to have the home birth after all! The midwives had given up, but we hadn’t.
“Appalachian Spring” was the first thing that popped up on the anesthesiologist’s phone. Would that song have been on our home birth playlist? As they continued to prep me for surgery, he explained the “curtain,” the shield to keep me from seeing everything that happened from the waist down. Since I worked for a theatre, we pretended the whole delivery was a stage production. But I’d written an entirely different play from the one we were performing.
A few hours earlier, we had celebrated the possibility of avoiding a hospital birth, as long as the baby stayed head down. Burgers in downtown Denton. Dark orange pee when I went to the bathroom. But the midwife texted back saying it was probably normal. Chocolate from the old-time candy shop. A funny warm, wet feeling. The candy shop girls said they didn’t have a bathroom. How dare they turn down the pregnant lady? We went next door to the visitors’ center. Blood. Definitely blood. And this time, the midwife texted back: not normal.
Appalachian Spring progressed through the movements: slowly, moderato, allegro. I couldn’t see what was going on. The anesthesiologist kept talking to me, I think, to distract me. I never felt the baby come out of me. I was numb from the waist down. Did a few seconds pass by? A few minutes? Muffled sounds.
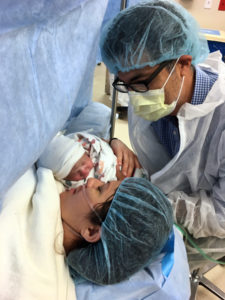
“Oh wow, she’s so beautiful,” I heard my husband say. Everything must be okay, then, I thought. Distant sounds of crying, nurses and doctors talking simultaneously. We were now onto the fourth movement of Appalachian Spring. Fast. Six pounds. Stern commands from the obstetrician to the operating team. Apgar score. I didn’t feel as if I were actually in the room, until she was plopped into my arms, cleaned up, swaddled in the standard hospital blanket, with a little hat.
Lucia was born four weeks before her due date, on May 31, 2017, at 9:29 PM, forced out of my womb with forceps through a C-section incision. Where were the gentle hands of the midwives?
I don’t have a clear memory of anything the rest of the night. I’ve spent hours looking through the photos and video that Daniel took, like an investigator, trying to piece together the clues to figure out what happened. Drunk from whatever narcotic they’d given me, as the effects of the spinal began to wear off, I rattled nonsense to the nurses. The last thing I remember was watching the ceiling spin before I passed out from exhaustion.
We knew there were risks to having an external cephalic version, including tearing of the placenta and preterm labor. But the risks were small. And I just happened to be on the wrong side of the statistics. If we hadn’t had the ECV, Lucia would have remained breech, and the obstetrician would have just delivered her naturally
Or maybe she would have turned head-down on her own. Or she wouldn’t have been breech in the first place if I’d stayed with an obstetrician the whole time. I’d read somewhere that babies were sometimes breech if the mothers were too anxious. Perhaps, no matter what I did, I would have had a C-section anyway. But at least, if we’d planned for it, I would have been able to pack a toothbrush and a pair of slippers.
